For millions of people living with major depressive disorder, antidepressant medications provide relief. But for a significant number of patients, symptoms persist despite trying multiple medications. This condition—commonly called medication-resistant or treatment-resistant depression—can feel discouraging and overwhelming.
Transcranial Magnetic Stimulation (TMS) offers a science-backed, non-invasive alternative for individuals who have not responded adequately to antidepressants. In this article, we’ll explain what TMS is, how it works, who it may help, and why it has become an increasingly important option in modern mental health care.
What Is Medication-Resistant Depression?
Medication-resistant depression (MRD) is typically defined as depression that does not significantly improve after trying two or more antidepressant medications, taken at appropriate doses for an adequate length of time.
People with MRD may experience:
- Persistent low mood or emotional numbness
- Fatigue and lack of motivation
- Difficulty concentrating or making decisions
- Sleep disturbances
- Loss of interest in previously enjoyed activities
When medications fail to provide relief—or cause intolerable side effects—patients and clinicians often look for alternative treatments.
What Is Transcranial Magnetic Stimulation (TMS)?
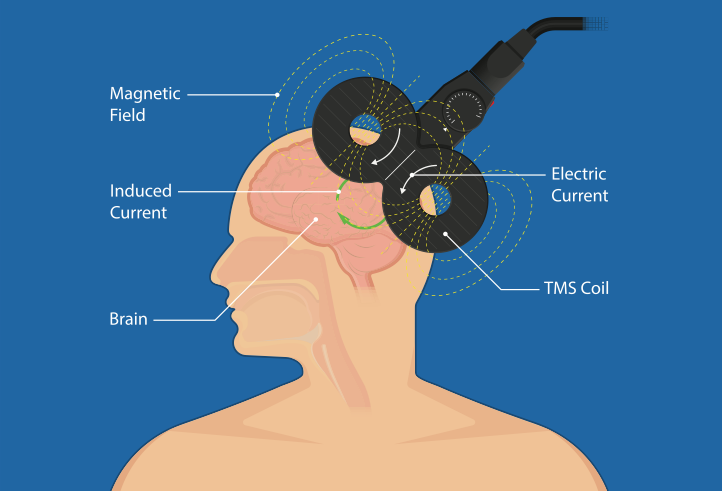
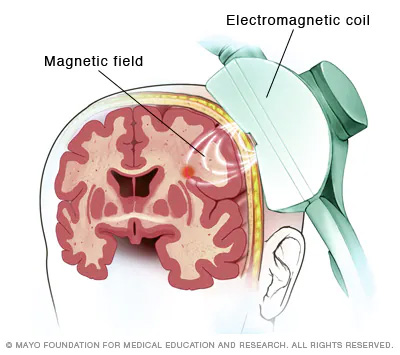
Transcranial Magnetic Stimulation (TMS) is a non-invasive outpatient procedure that uses focused magnetic pulses to stimulate specific areas of the brain involved in mood regulation, particularly the left dorsolateral prefrontal cortex.
TMS does not require:
- Surgery
- Anesthesia
- Sedation
- Systemic medication
It is cleared by the U.S. Food and Drug Administration for the treatment of major depressive disorder in patients who have not responded to antidepressant medications.
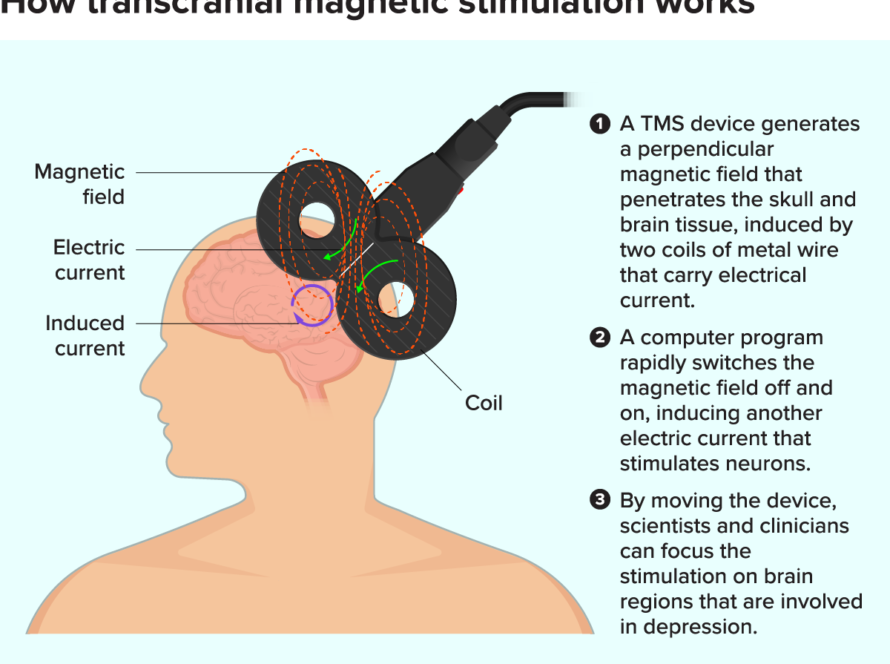
How Does TMS Work for Depression?
Depression is associated with reduced activity in certain brain circuits responsible for mood, motivation, and executive function. TMS delivers magnetic pulses that painlessly pass through the scalp and skull, inducing small electrical currents in targeted brain tissue.
Over time, these repeated stimulations can:
- Increase activity in underactive mood-related regions
- Improve communication between neural networks
- Promote neuroplasticity (the brain’s ability to adapt and rewire)
Unlike medications, which affect the entire body, TMS is precisely targeted, which is why it tends to have fewer systemic side effects.
What to Expect During TMS Treatment
A typical TMS treatment course includes:
- Sessions 5 days per week
- Each session lasting about 20–40 minutes
- A total treatment course of 4–6 weeks
During treatment:
- You remain awake and alert
- A coil is placed gently against your head
- You may feel a tapping sensation on the scalp
Most patients return to work or daily activities immediately after each session.
Is TMS Effective for Medication-Resistant Depression?
Clinical studies and real-world outcomes consistently show that TMS can significantly reduce depressive symptoms in patients who have not responded to medication alone.
Many patients experience:
- Improved mood
- Increased energy and motivation
- Better concentration
- Reduced feelings of hopelessness
For some individuals, TMS leads to full remission of depressive symptoms; for others, it provides meaningful improvement and improved quality of life.
Safety and Side Effects of TMS
TMS is widely regarded as a safe and well-tolerated treatment. The most common side effects are mild and temporary, including:
- Scalp discomfort or headache during early sessions
- Mild jaw or facial muscle twitching
Serious side effects are rare, and TMS does not cause memory loss or cognitive impairment—an important distinction from some other brain-based treatments.
Who Is a Good Candidate for TMS?
TMS may be appropriate for adults who:
- Have been diagnosed with major depressive disorder
- Have not responded adequately to antidepressant medications
- Cannot tolerate medication side effects
- Prefer a non-drug, non-invasive treatment option
A consultation with a qualified medical provider is essential to determine candidacy and tailor the treatment plan.
Why TMS Is an Important Option in Modern Depression Care
Medication-resistant depression is more common than many people realize, and it does not mean that recovery is out of reach. TMS represents a shift toward precision-based, neuroscience-driven mental health care, offering hope where traditional treatments fall short.
As awareness grows and access expands, TMS is becoming a cornerstone therapy for patients seeking effective, evidence-based relief from depression.
Frequently Asked Questions About TMS for Depression
Is TMS covered by insurance?
Many insurance plans, including Medicare, cover TMS for treatment-resistant depression when medical criteria are met.
How long do results last?
Many patients experience long-lasting benefits. Some may choose occasional maintenance sessions if symptoms return.
Does TMS replace medication?
In some cases, yes. In others, TMS is used alongside medication as part of a comprehensive treatment plan.
Final Thoughts
If you or a loved one is struggling with depression that hasn’t improved with medication, Transcranial Magnetic Stimulation may offer a safe, effective, and life-changing alternative. By directly targeting the brain circuits involved in mood regulation, TMS opens new possibilities for recovery and renewed quality of life.
Always consult with a qualified healthcare provider to determine the most appropriate treatment for your individual needs.